A CHOC expert discusses the most common pediatric orthpaedic injuries and cancers and how they’re treated and diagnosed.
Virtual Pediatric Lecture Series: Pediatric Orthopaedics
CHOC’s virtual pediatric lecture series continues with “Pediatric orthopaedics: Buckle fractures, osteosarcoma and some things in between.”
Recent Advancements Shape the Future of Sarcoma Care
At CHOC, collaborative research, experimental treatment protocols & surgical advancements are setting the stage to change sarcoma treatment.
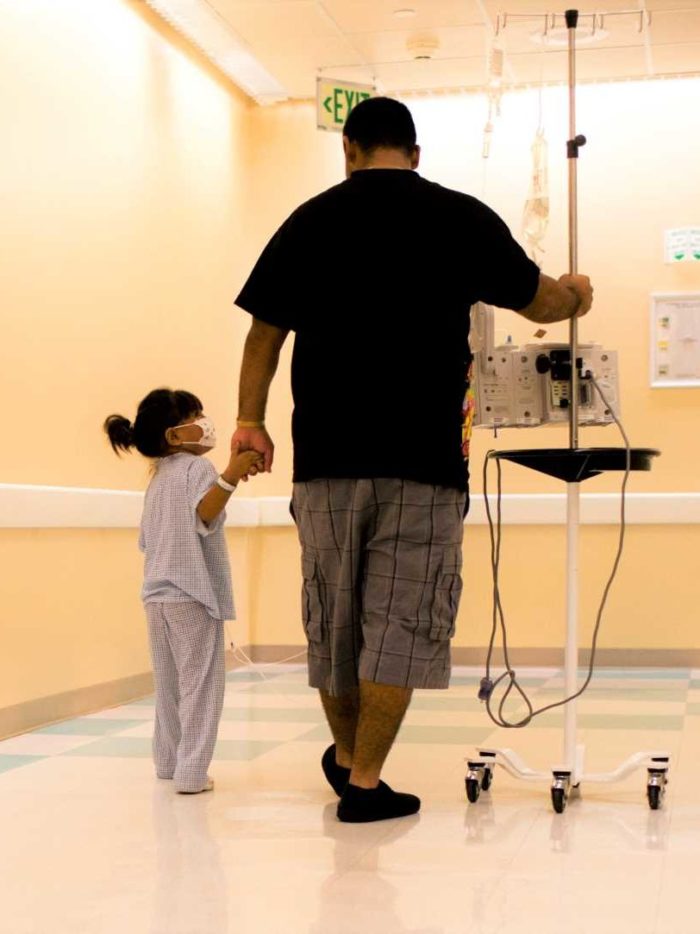
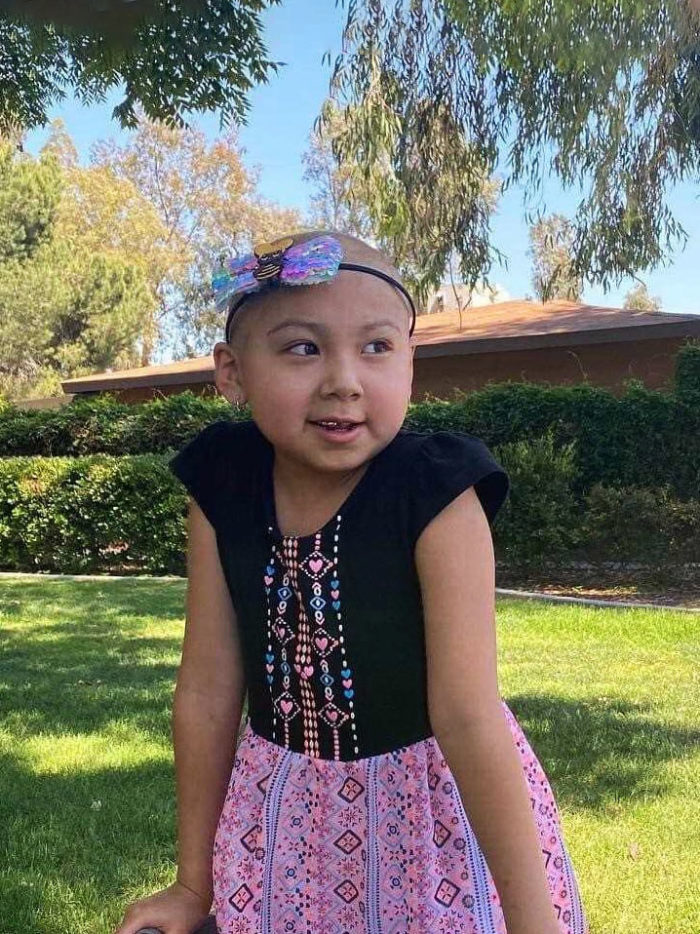
Cutting-edge device approved for compassionate use saves leg, life of cancer patient
Naomi’s story highlights CHOC’s commitment to innovation in patient care, including investigational therapies, diagnostics and devices.
IN THE SPOTLIGHT: Dr. Amir Misaghi
Dr. Amir Misaghi shares why he decided to become a doctor, new developments in his field, his hobbies outside of work and more.