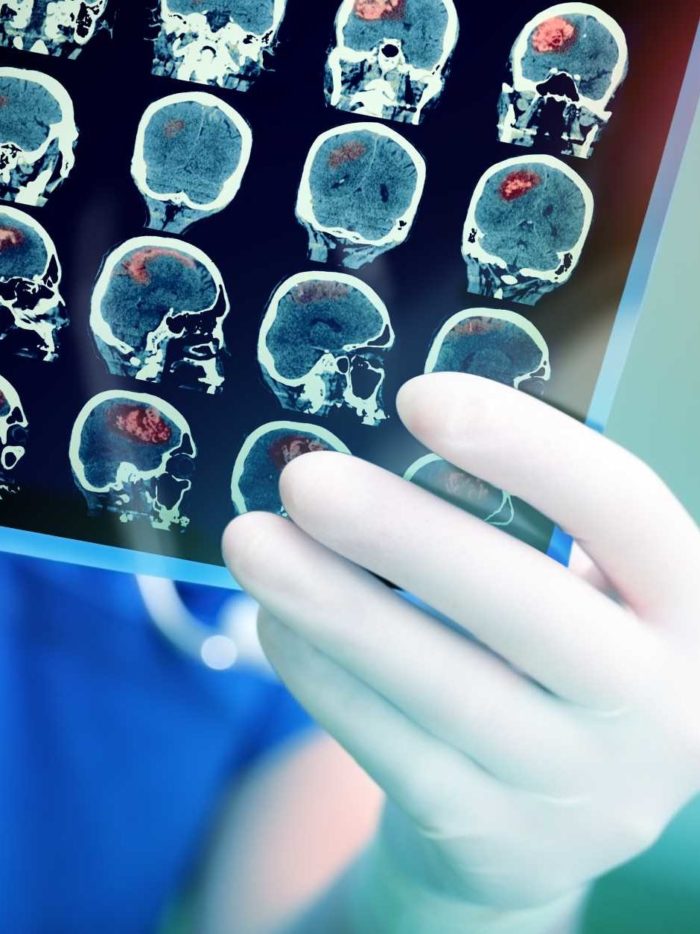
A year after undergoing laser interstitial thermal therapy, a young patient showed significant reduction in tumor size and enhancement.
Personalized medicine, surgical innovations advance pediatric brain tumor care
The Neuro-Oncology Treatment Program at CHOC is helping to shape the future of personalized medicine and surgical innovations.
In the Spotlight: Chenue Abongwa, M.D.
Chenue Abongwa, M.D., joined CHOC in October 2018 as a pediatric neuro-oncologist at the Hyundai Cancer Institute.