A CHOC expert in sports medicine offers strategies to pediatricians for successfully diagnosing, referring and treating sports injuries.
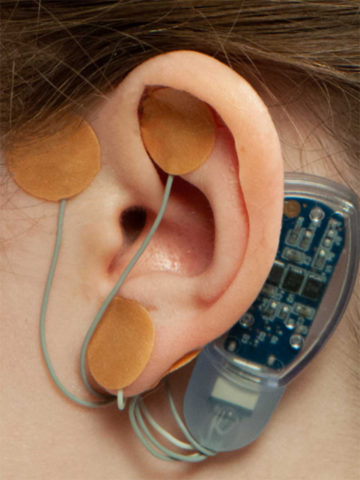
Device for patients with GI issues showing promise in treating Post-Concussion Syndrome
CHOC doctors discover the possible efficacy of treating PCS with the GI device IB-Stim. A clinical trial is underway.
Clearing pediatric patients for sports after COVID-19: Tips for pediatricians
CHOC experts share what providers ought to know when clearing young athletes for a return to sports following a COVID-19 infection.
Return to Learn Concussion Guidelines Every Medical Provider Should Know
When returning a student to the classroom after a concussion, practitioners try to balance stimulation levels and worsening of symptoms.