Dr. Buethe aims to develop a comprehensive, one-stop center for children and adolescents with complex skin, hair and nail disorders.
Planning the future together: CHOC Research Institute welcomes Rady at 2025 strategy retreat
The annual conference signals a new era under the Rady Children’s Health umbrella.
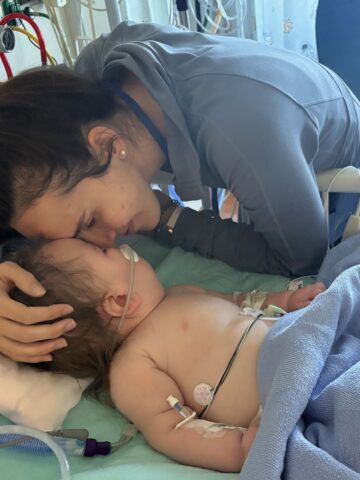
Parents of 1-year-old with exceedingly rare and life-threatening mitochondrial disease entrust CHOC above anywhere else
With time not on their side, CHOC care team pulls out all stops to save life of Emery Kline.
Novel bioelectronic device could advance pediatric neurologic care
Learn how a CHOC clinician helped develop a bioelectronic implant that could, one day, improve brain signal monitoring in children with neurologic disorders.
Experts address the most pressing challenges at Pediatric & Lifespan Data Science Conference
Panel discussions also were held on precision medicine, fairness in AI, precision management of psychiatric conditions, and other issues.
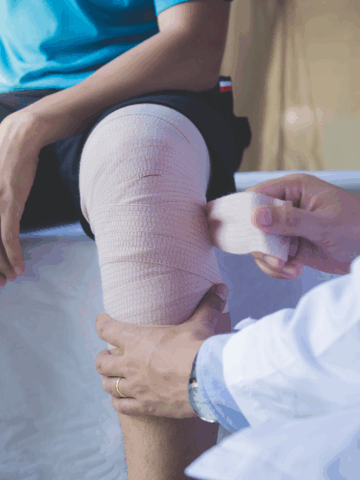
CHOC research finds severity of e-bike pediatric orthopedic injuries comparable to motor vehicle accidents
Electric bicycles (e-bikes) are faster and easier to pedal than traditional bikes, making them increasingly popular with teens and young adults. Along with a rise in popularity, physicians at CHOC are witnessing a surge in e-bike injuries. Dr. John Schlechter, pediatric orthopedic surgeon specializing in sports medicine, arthroscopy, and fracture care for children and adolescents […]