A first-of-its-kind study by CHOC found that awareness and safety precautions are vital to prevent severe injuries from mechanic bull riding.
New tool for craniosynostosis treatment highlights Neuroscience Institute’s push to advance care
A recently installed 3D camera system in CHOC’s neurosurgery clinic will significantly advance CHOC’s mission to treat craniosynostosis.
First batch of awardees announced for new Chief Scientific Officer small grant program
Research projects of the winners – 12 of 23 were awarded funding – range from virtual reality training to the use of AI to predict COVID-19.
Neuroscience leaders discuss innovations and their successes, and the need for much more work to be done
Neurosurgeons share their insights on how innovation is closing the gap between clinical needs and the availability of pediatric devices.
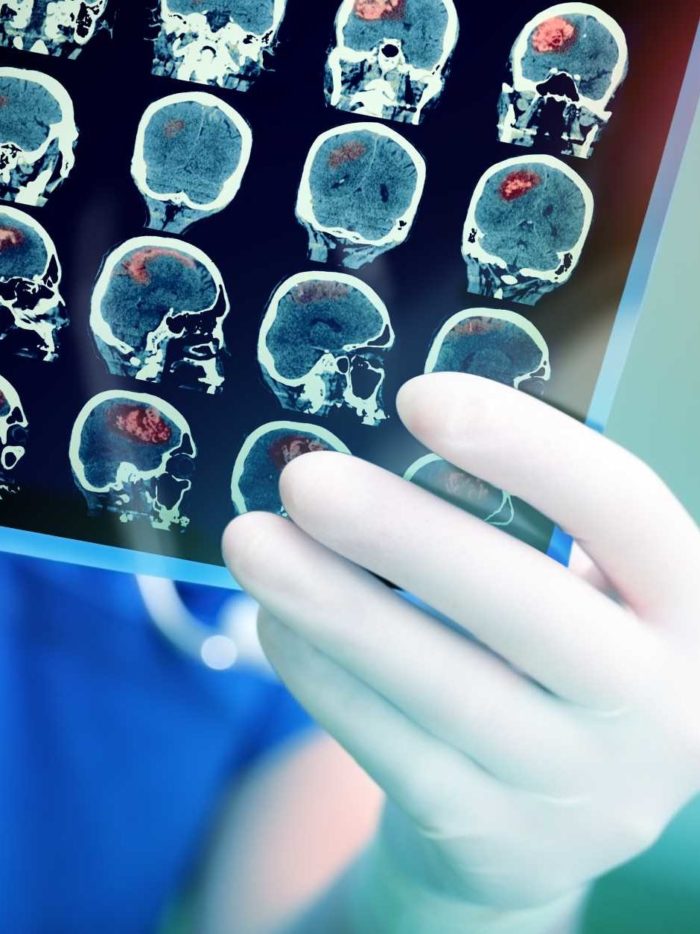
Personalized medicine, surgical innovations advance pediatric brain tumor care
The Neuro-Oncology Treatment Program at CHOC is helping to shape the future of personalized medicine and surgical innovations.
I’m a pediatric neurosurgeon. Here’s why I’m excited about the technology at our fingertips.
Dr. Suresh Magge, medical director of neurosurgery at CHOC, discusses four surgeries he is excited about as a pediatric neurosurgeon.