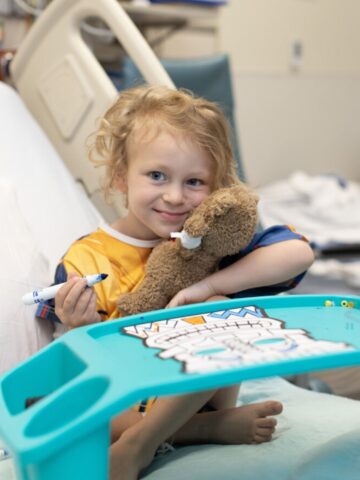
Navigating from child to young adult can be very challenging in the best of circumstances.
Add a chronic or rare medical condition to the journey, and the process can get very scary.
Teens with chronic conditions face a higher risk of non-adherence to taking their medication or even obtaining it when transitioning from a pediatric to adult primary care provider, medical experts say. And statistically, the chance of them having to be admitted into an ER or have surgery increases, as does the prospect of them dropping out of treatment – which could have fatal results.
Dr. Mary L. Zupanc, co-medical director of CHOC’s Neuroscience Institute and a pediatric neurologist who specializes in epilepsy and rare conditions, stressed in a recent webinar that she’s passionate about preventing patients transitioning to adult care from falling through the cracks.

“We begin with introducing the concept of transitioning to adult care when our patients are 12 years old,” Dr. Zupanc said while speaking on a four-person panel hosted by Global Genes, an Aliso Viejo-based non-profit that advocates for the rare disease community.
The topic of the 50-minute discussion on Sept. 24, 2020 was “Navigating the Transition of Care for Young Adult Patients.”
In addition to her position at CHOC and as a faculty member at UC Irvine, Dr. Zupanc sits on the board of directors of the Child Neurology Foundation (CNF) in Minneapolis, Minn. On its website, the CNF details several resources about transitioning to adult care.
“We at CHOC have followed the CNF’s template to develop a formal transitioning program here,” Dr. Zupanc said.
Starting the conversation with families when a patient is 12 years old may seem too early, Dr. Zupanc said. But transitioning is a process that doesn’t have a one-size-fits-all solution, and it’s critical to start the discussion when patients are young.
The other panelists agreed. They were Dr. Leah Ratner, a fellow at Brigham and Women’s Hospital in Boston; Sneha Dave, 22, a student at Indiana University who since age 6 has lived with ulcerative colitis; and moderator Amy Ohmer, director of the International Children’s Advisory Network in Marietta, Ga., and the mother of two daughters, ages 17 and 19, who have chronic and rare conditions.
“I think it’s important to introduce the concept (of transitioning) early – to let the parents and patient know, ‘We’re not just going to throw you out,’” Dr. Zupanc said. “Rather, ‘We’re going to work with you so you can learn to self-manage your disease and your medications. And we’re going to go over your plan on a yearly or bi-annual basis.’”
Under the transitioning plan adopted by CHOC thanks to a grant, a healthcare transition program is initiated when patients turn 12 years of age.
Clinicians, social workers, and others continue to prepare their patients and their families for increased independence and management of their care, as well as to the adult model of care, Dr. Zupanc explained.
The actual transition to adult care varies from 18 to 22 years of age—often dependent on insurance—and ideally occurs in stages, as these young adults may have multiple subspecialists. Between the ages of 23 and 26 years, the young adults are integrated into adult care.
“It’s a partnership,” Dr. Zupanc said. “It takes a community.”
Sneha, the Indiana University student, said the transition must go slow because there are so many components to it, such as having to navigate health insurance.
“Young adults diagnosed with a condition at childhood tend not to be as prepared because their parents or guardians took care of everything and they had no ownership of their own care,” Sneha said.
When she was a freshman, Sneha founded the Health Advocacy Summit, which empowers young adults with chronic and rare diseases through advocacy events and programs. In August 2020, the organization hosted an international virtual summit.
“It’s a process,” Dr. Zupanc agreed of transitioning to adult care. “And I think it’s a process of self-empowerment. Most parents are used to taking care of everything. We try to empower our teenager and young adults as much as possible. Parents have to let go at some point, but it’s a process.”
The bulk of Dr. Zupanc’s patients have severe epilepsy that started in infancy. A high percentage also have intellectual disabilities.
“Sometimes they take a step forward and two steps back,” she said.
The path toward a successful transition to adult care begins with knowledge, she explained, followed by support, confidence and, finally, independence.
Dr. Zupanc noted that patients who leave CHOC are welcomed to stay in touch.
“As a pediatric provider for children with rare diseases,” she said, “I let my families and adolescents know that I have their backs and that I’m not going to let them fall into the abyss. If there are issues, I’m here to help them.”
November is epilepsy awareness month. To learn more about CHOC’s Comprehensive Epilepsy Program, click here.